Enable sidebar
Off
All videos
-
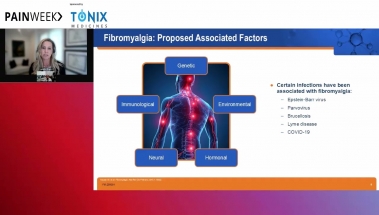
| fibromyalgia
-
Sep 30, 2025 -

Jun 9, 2025 -

Apr 8, 2025 -

Apr 7, 2025 -

Apr 1, 2025 -

Mar 1, 2025 -

Feb 3, 2025 -

Jan 2, 2025

